Cornea Transplant
Corneal Transplant: Overview
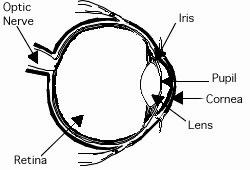
The cornea is the eye’s outermost layer. It is the clear, dome-shaped surface that covers the front of the eye. The cornea helps focus light as it passes through the eye. An unhealthy cornea can distort and cloud vision. Permanent damage to the cornea may require a cornea transplant.
Printable Version (PDF)
What is a corneal transplant? Is it safe?
A corneal transplant involves replacing a diseased or scarred cornea with a new one. When the cornea becomes cloudy, light cannot penetrate the eye to reach the light-sensitive retina. Poor vision or blindness may result.
The first step in a corneal transplant is to find a donor cornea. Your name and information will be logged into a donor database and you will be notified when a match is made. The wait is usually short. The donated cornea is thoroughly tested for infectious disease, and for its visual correction capabilities.
In corneal transplant surgery, the surgeon removes the central portion of the cloudy cornea and replaces it with a clear cornea, usually donated through an eye bank. A trephine, an instrument like a cookie cutter, is used to remove the cloudy cornea. The surgeon places the new cornea in the opening and sews it with a very fine thread. The thread stays in for months or even years until the eye heals properly (removing the thread is quite simple and can easily be done in an ophthalmologist’s office). Following surgery, eye drops to help promote healing will be needed for several months. Most patients return home the same day of surgery. Someone else will need to drive you home after the procedure.
Corneal transplants are very common in the United States; about 40,000 are performed each year. The chances of success of this operation have risen dramatically because of technological advances, such as less irritating sutures or threads, which are often finer than a human hair; and the surgical microscope. Corneal transplantation has restored sight to many who, a generation ago, would have been blinded permanently by corneal injury, infection, or inherited corneal disease or degeneration.
What problems can develop from a corneal transplant?
Even with a fairly high success rate, some problems can develop, such as rejection of the new cornea. Warning signs for rejection are decreased vision, increased redness of the eye, increased pain, and increased sensitivity to light. If any of these last for more than six hours, you should immediately call your ophthalmologist. Rejection can be successfully treated if medication is administered at the first sign of symptoms.
A study supported by the National Eye Institute (NEI) suggests that matching the blood type, but not tissue type, of the recipient with that of the cornea donor may improve the success rate of corneal transplants in people at high risk for graft failure. Approximately 20 percent of corneal transplant patients – between 6000-8000 a year – reject their donor corneas. The NEI-supported study found that high-risk patients may reduce the likelihood of corneal rejection if their blood types match those of the cornea donors. The study also concluded that intensive steroid treatment after transplant surgery improves the chances for a successful transplant.
Are there alternatives to a corneal transplant?
Phototherapeutic keratectomy (PTK) is one of the latest advances in eye care for the treatment of corneal dystrophies, corneal scars, and certain corneal infections. Only a short time ago, people with these disorders would most likely have needed a corneal transplant. By combining the precision of the excimer laser with the control of a computer, doctors can vaporize microscopically thin layers of diseased corneal tissue and etch away the surface irregularities associated with many corneal dystrophies and scars. Surrounding areas suffer relatively little trauma. New tissue can then grow over the now-smooth surface. Recovery from the procedure takes a matter of days, rather than months as with a transplant. The return of vision can occur rapidly, especially if the cause of the problem is confined to the top layer of the cornea. Studies have shown close to an 85 percent success rate in corneal repair using PTK for well-selected patients.
This educational material is provided by Dialog Medical.
© Copyright 2005 Dialog Medical
All Rights Reserved
The Eye Center
Call Toll Free 1.888.844.2020

