Glaucoma
Glaucoma: Overview
Printable Version (PDF)
This information is designed to help people with glaucoma and their families better understand the disease. It describes the causes, symptoms, diagnosis, and treatment of glaucoma. It is mainly about open-angle glaucoma, the most common kind in the United States.
Glaucoma is a group of diseases that can lead to damage to the eye’s optic nerve and result in blindness.
Open-angle glaucoma, the most common form of glaucoma, affects about 3 million Americans–half of whom don’t know they have it. It has no symptoms at first. But over the years it can steal your sight. With early treatment, you can often protect your eyes against serious vision.
What is the optic nerve?
The optic nerve is a bundle of more than 1 million nerve fibers. It connects the retina, the light-sensitive layer of tissue at the back of the eye, with the brain (see diagram). A healthy optic nerve is necessary for good vision.
How does glaucoma damage the optic nerve?
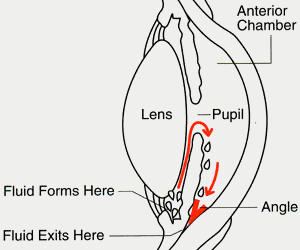
In many people, increased pressure inside the eye causes glaucoma. In the front of the eye is a space called the anterior chamber. A clear fluid flows continuously in and out of this space and nourishes nearby tissues.
The fluid leaves the anterior chamber at the angle where the cornea and iris meet (see diagram). When the fluid reaches the angle, it flows through a spongy meshwork, like a drain, and leaves the eye.
Open-angle glaucoma gets its name because the angle that allows fluid to drain out of the anterior chamber is open. However, for unknown reasons, the fluid passes too slowly through the meshwork drain. As the fluid builds up, the pressure inside the eye rises. Unless the pressure at the front of the eye is controlled, it can damage the optic nerve and cause vision loss.
Who is at risk?
Although anyone can get glaucoma, some people are at higher risk than others. They include:
- Blacks over age 40
- Everyone over age 60
- People with a family history of glaucoma.
What are the symptoms of glaucoma?
At first, open-angle glaucoma has no symptoms. Vision stays normal, and there is no pain. As glaucoma remains untreated, people may notice that although they see things clearly in front of them, they miss objects to the side and out of the corner of their eye.
Without treatment, people with glaucoma may find that they suddenly have no side vision. It may seem as though they are looking through a tunnel. Over time, the remaining forward vision may decrease until there is no vision left.
How is glaucoma detected?
Most people think that they have glaucoma if the pressure in their eye is increased. This is not always true. High pressure puts you at risk for glaucoma. It may not mean that you have the disease.
Whether or not you get glaucoma depends on the level of pressure that your optic nerve can tolerate without being damaged. This level is different for each person.

View of boys by person with normal vision.

View of boys by person with glaucoma.
Although normal pressure is usually between 12-21 mm Hg, a person might have glaucoma even if the pressure is in this range. That is why an eye examination is very important.
To detect glaucoma, your eye care professional will do the following tests:
- Visual acuity: This eye chart test measures how well you see at various distances.
- Visual Field: This test measures your side (peripheral) vision. It helps your eye care professional find out if you have lost side vision, a sign of glaucoma.
- Pupil dilation: This examination provides your eye care professional with a better view of the optic nerve to check for signs of damage. To do this, your eye care professional places drops into the eye to dilate (widen) the pupil. After the examination, your close-up vision may remain blurred for several hours.
- Tonometry: This standard test determines the fluid pressure inside the eye. There are many types of tonometry. One type uses a purple light to measure pressure. Another type is the “air puff,” test, which measures the resistance of the eye to a puff of air.
Can glaucoma be treated?
Yes. Although you will never be cured of glaucoma, treatment often can control it. This makes early diagnosis and treatment important to protect your sight. Most doctors use medications for newly diagnosed glaucoma; however, new research findings show that laser surgery is a safe and effective alternative.
Glaucoma treatments include:
Medicine: Medicines are the most common early treatment for glaucoma. They come in the form of eyedrops and pills. Some cause the eye to make less fluid. Others lower pressure by helping fluid drain from the eye.
Glaucoma drugs may be taken several times a day. Most people have no problems. However, some medicines can cause headaches or have side effects which affect other parts of the body. Drops may cause stinging, burning, and redness in the eye. Ask your eye care professional to show you how to put the drops into your eye. In addition, tell your eye care professional about other medications you may be taking before you begin glaucoma treatment.
Many drugs are available to treat glaucoma. If you have problems with one medication, tell your eye care professional. Treatment using a different dosage or a new drug may be possible.
You will need to use the drops and/or pills as long as they help to control your eye pressure. This is very important. Because glaucoma often has no symptoms, people may be tempted to stop or may forget to take their medicine.
Laser surgery (also called laser trabeculoplasty): Laser surgery helps fluid drain out of the eye. Although your eye care professional may suggest laser surgery at any time, it is often done after trying treatment with medicines. In many cases, you will need to keep taking glaucoma drugs even after laser surgery.
Laser surgery is performed in an eye care professional’s office or eye clinic. Before the surgery, your eye care professional will apply drops to numb the eye.
As you sit facing the laser machine, your eye care professional will hold a special lens to your eye. A high-energy beam of light is aimed at the lens and reflected onto the meshwork inside your eye. You may see flashes of bright green or red light. The laser makes 50-100 evenly spaced burns. These burns stretch the drainage holes in the meshwork. This helps to open the holes and lets fluid drain better through them.
Your eye care professional will check your eye pressure shortly afterward. He or she may also give you some drops to take home for any soreness or swelling inside the eye. You will need to make several followup visits to have your pressure monitored.
Once you have had laser surgery over the entire meshwork, further laser treatment may not help. Studies show that laser surgery is very good at getting the pressure down. But its effects sometimes wear off over time. Two years after laser surgery, the pressure increases again in more than half of all patients.
Conventional surgery: The purpose of surgery is to make a new opening for the fluid to leave the eye. Although your eye care professional may suggest it at any time, this surgery is often done after medicine and laser surgery have failed to control your pressure.
Surgery is performed in a clinic or hospital. Before the surgery, your eye care professional gives you medicine to help you relax and then small injections around the eye to make it numb.
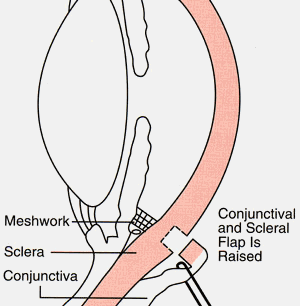
The eye care professional removes a small piece of tissue from the white (sclera) of the eye. This creates a new channel for fluid to drain from the eye. But surgery does not leave an open hole in the eye. The white of the eye is covered by a thin, clear tissue called the conjunctiva. The fluid flows through the new opening, under the conjunctiva, and drains from the eye.
You must put drops in the eye for several weeks after the operation to fight infection and swelling. (The drops will be different than the eyedrops you were using before surgery.) You will also need to make frequent visits to your eye care professional. This is very important, especially in the first few weeks after surgery.
In 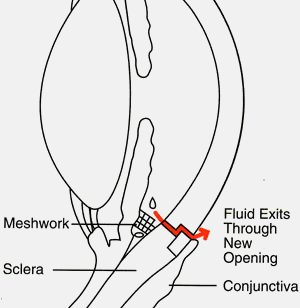
Keep in mind that while glaucoma surgery may save remaining vision, it does not improve sight. In fact, your vision may not be as good as it was before surgery.
Like any operation, glaucoma surgery can cause side effects. These include cataract, problems with the cornea, inflammation or infection inside the eye, and swelling of blood vessels behind the eye. However, if you do have any of these problems, effective treatments are available.
What are some other forms of glaucoma?
Although open-angle glaucoma is the most common form, some people have other forms of the disease.
In low-tension or normal-tension glaucoma, optic nerve damage and narrowed side vision occur unexpectedly in people with normal eye pressure. People with this form of the disease have the same types of treatment as open-angle glaucoma.
In closed-angle glaucoma, the fluid at the front of the eye cannot reach the angle and leave the eye because the angle gets blocked by part of the iris. People with this type of glaucoma have a sudden increase in pressure. Symptoms include severe pain and nausea as well as redness of the eye and blurred vision. This is a medical emergency. The patient needs immediate treatment to improve the flow of fluid. Without treatment, the eye can become blind in as little as one or two days. Usually, prompt laser surgery can clear the blockage and protect sight.
In congenital glaucoma, children are born with defects in the angle of the eye that slow the normal drainage of fluid. Children with this problem usually have obvious symptoms such as cloudy eyes, sensitivity to light, and excessive tearing. Surgery is usually the suggested treatment, because medicines may have unknown effects in infants and be difficult to give to them. The surgery is safe and effective. If surgery is done promptly, these children usually have an excellent chance of having good vision.
Secondary glaucomas can develop as a complication of other medical conditions. They are sometimes associated with eye surgery or advanced cataracts, eye injuries, certain eye tumors, or uveitis (eye inflammation). One type, known as pigmentary glaucoma, occurs when pigment from the iris flakes off and blocks the meshwork, slowing fluid drainage. A severe form, called neovascular glaucoma, is linked to diabetes. Also, corticosteroid drugs used to treat eye inflammations and other diseases–can trigger glaucoma in a few people. Treatment is with medicines, laser surgery, or conventional surgery.
What research is being done?
The National Eye Institute (NEI) is the Federal government’s lead agency for vision research. The NEI is supporting many research studies both in the laboratory and with patients. This research should provide better ways in the future to detect, treat, and prevent vision loss in people with glaucoma.
For instance, researchers recently found a gene that causes a form of glaucoma that starts at a young age. This is the first glaucoma gene ever located. This finding could help us learn more about how glaucoma damages the eye.
The NEI is also supporting clinical studies that will tell us more about who is likely to get glaucoma, when to treat people with increased pressure, and which treatment to use first.
What can you do to protect your vision?
If you are being treated for glaucoma, be sure to take your glaucoma medicine every day and see your eye care professional regularly.
You can also help protect the vision of family members and friends who may be at high risk for glaucoma–Blacks over age 40 and everyone over age 60. Encourage them to have an eye examination through dilated pupils every two years.
For more information about glaucoma, you may wish to contact:
American Academy of Ophthalmology
655 Beach Street
San Francisco, CA 94109-7424
(415) 561-8500
http://www.eyenet.org
American Optometric Association
243 Lindbergh Boulevard
St. Louis, MO 63141
(314) 991-4100
AmOptCCC@aol.com
http://www.aoanet.org
(The) Glaucoma Foundation
33 Maiden Lane
New York, NY 10038
1-800-452-8266
(212) 285-0080
glaucomafdn@mindspring.com
http://www.glaucoma-foundation.org
Glaucoma Research Foundation
200 Pine Street, Suite 200
San Francisco, CA 94104
1-800-826-6693
(415) 986-3162
http://www.glaucoma.org
National Eye Institute
2020 Vision Place
Bethesda, MD 20892-3655
(301) 496-5248
2020@nei.nih.gov
http://www.nei.nih.gov
Prevent Blindness America
500 East Remington Road
Schaumburg, IL 60173
1 (800) 331 -2020
(847) 843-2020
http://prevent-blindness.org
National Eye Institute
National Institutes of Health
NIH Publication No. 99-651
April 2000
This educational material is provided by Dialog Medical.
© Copyright 2005 Dialog Medical
All Rights Reserved
The Eye Center
Call Toll Free 1.888.844.2020