Diabetic Retinopathy
This pamphlet has been written to help people with diabetic retinopathy and their families and friends better understand the disease. It describes the cause, symptoms, diagnosis, and treatment of diabetic retinopathy.
Diabetic retinopathy is a potentially blinding complication of diabetes that damages the eye’s retina. It affects half of all Americans diagnosed with diabetes.
At first, you may notice no changes in your vision. But don’t let diabetic retinopathy fool you. It could get worse over the years and threaten your good vision. With timely treatment, 90 percent of those with advanced diabetic retinopathy can be saved from going blind.
The National Eye Institute (NEI) is the Federal government’s lead agency for vision research. The NEI urges all people with diabetes to have an eye examination through dilated pupils at least once a year.
What is the retina?
The retina is a light-sensitive tissue at the back of the eye. When light enters the eye, the retina changes the light into nerve signals. The retina then sends these signals along the optic nerve to the brain. Without a retina, the eye cannot communicate with the brain, making vision impossible.
Printable Version (PDF)
How does diabetic retinopathy damage the retina?
Diabetic retinopathy occurs when diabetes damages the tiny blood vessels in the retina. At this point, most people do not notice any changes in their vision.
Some people develop a condition called macular edema. It occurs when the damaged blood vessels leak fluid and lipids onto the macula, the part of the retina that lets us see detail. The fluid makes the macula swell, blurring vision.
As the disease progresses, it enters its advanced, or proliferative, stage. Fragile, new blood vessels grow along the retina and in the clear, gel-like vitreous that fills the inside of the eye. Without timely treatment, these new blood vessels can bleed, cloud vision, and destroy the retina.
Who is at risk for this disease?
All people with diabetes are at risk–those with Type I diabetes (juvenile onset) and those with Type II diabetes (adult onset).
During pregnancy, diabetic retinopathy may also be a problem for women with diabetes. It is recommended that all pregnant women with diabetes have dilated eye examinations each trimester to protect their vision.
What are its symptoms?
Diabetic retinopathy often has no early warning signs. At some point, though, you may have macular edema. It blurs vision, making it hard to do things like read and drive. In some cases, your vision will get better or worse during the day.

View of boys by person with normal vision.

View of boys by person with diabetic retinopathy.
As new blood vessels form at the back of the eye, they can bleed (hemorrhage) and blur vision. The first time this happens it may not be very severe. In most cases, it will leave just a few specks of blood, or spots, floating in your vision. They often go away after a few hours.
These spots are often followed within a few days or weeks by a much greater leakage of blood. The blood will blur your vision. In extreme cases, a person will only be able to tell light from dark in that eye. It may take the blood anywhere from a few days to months or even years to clear from the inside of your eye. In some cases, the blood will not clear. You should be aware that large hemorrhages tend to happen more than once, often during sleep.
How is it detected?
Diabetic retinopathy is detected during an eye examination that includes:
Visual acuity test: This eye chart test measures how well you see at various distances.
Pupil dilation:The eye care professional places drops into the eye to widen the pupil. This allows him or her to see more of the retina and look for signs of diabetic retinopathy. After the examination, close-up vision may remain blurred for several hours.
Ophthalmoscopy:This is an examination of the retina in which the eye care professional: (1) looks through a device with a special magnifying lens that provides a narrow view of the retina, or (2) wearing a headset with a bright light, looks through a special magnifying glass and gains a wide view of the retina.
Tonometry: A standard test that determines the fluid pressure inside the eye. Elevated pressure is a possible sign of glaucoma, another common eye problem in people with diabetes.
Your eye care professional will look at your retina for early signs of the disease, such as: (1) leaking blood vessels, (2) retinal swelling, such as macular edema, (3) pale, fatty deposits on the retina–signs of leaking blood vessels, (4) damaged nerve tissue, and (5) any changes in the blood vessels.
Should your doctor suspect that you need treatment for macular edema, he or she may ask you to have a test called fluorescein angiography.
In this test, a special dye is injected into your arm. Pictures are then taken as the dye passes through the blood vessels in the retina. This test allows your doctor to find the leaking blood vessels.
How is it treated?
There are two treatments for diabetic retinopathy. They are very effective in reducing vision loss from this disease. In fact, even people with advanced retinopathy have a 90 percent chance of keeping their vision when they get treatment before the retina is severely damaged.
These two treatments are laser surgery and vitrectomy. It is important to note that although these treatments are very successful, they do not cure diabetic retinopathy.
Laser Surgery
Laser surgery is performed in a doctor’s office or eye clinic. Before the surgery, your ophthalmologist will: (1) dilate your pupil and (2) apply drops to numb the eye. In some cases, the doctor also may numb the area behind the eye to prevent any discomfort.
The lights in the office will be dim. As you sit facing the laser machine, your doctor will hold a special lens to your eye. During the procedure, you may see flashes of light. These flashes may eventually create a stinging sensation that makes you feel a little uncomfortable.
You may leave the office once the treatment is done, but you will need someone to drive you home. Because your pupils will remain dilated for a few hours, you also should bring a pair of sunglasses.
For the rest of the day, your vision will probably be a little blurry. If your eye hurts a bit, your eye care professional can suggest a way to control this.

The retina immediately after focal laser treatment.
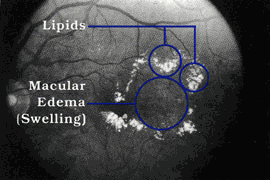
The retina prior to focal laser treatment.
Doctors will perform laser surgery to treat severe macular edema and proliferative retinopathy.
Macular Edema: Timely laser surgery can reduce vision loss from macular edema by half. But you may need to have laser surgery more than once to control the leaking fluid.
During the surgery, your doctor will aim a high-energy beam of light directly onto the damaged blood vessels. This is called focal laser treatment. This seals the vessels and stops them from leaking. Generally, laser surgery is used to stabilize vision, not necessarily to improve it.
Proliferative Retinopathy: In treating advanced diabetic retinopathy, doctors use the laser to destroy the abnormal blood vessels that form at the back of the eye.
Rather than focus the light on a single spot, your eye care professional will make hundreds of small laser burns away from the center of the retina. This is called scatter laser treatment. The treatment shrinks the abnormal blood vessels. You will lose some of your side vision after this surgery to save the rest of your sight. Laser surgery may also slightly reduce your color and night vision.
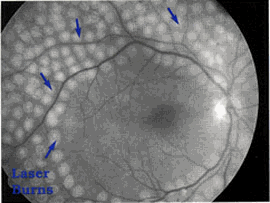
Scatter laser treatment.
Once you have proliferative retinopathy, you will always be at risk for new bleeding. This means you may need treatment more than once to protect your sight.
Vitrectomy
Instead of laser surgery, you may need an eye operation called a vitrectomy to restore your sight. A vitrectomy is performed if you have a lot of blood in the vitreous. It involves removing the cloudy vitreous and replacing it with a salt solution. Because the vitreous is mostly water, you will notice no change between the salt solution and the normal vitreous.
Studies show that people who have a vitrectomy soon after a large hemorrhage are more likely to protect their vision than someone who waits to have the operation.
Early vitrectomy is especially effective in people with insulin-dependent diabetes, who may be at greater risk of blindness from a hemorrhage into the eye.
Vitrectomy is often done under local anesthesia. This means that you will be awake during the operation. The doctor makes a tiny incision in the sclera, or white of the eye. Next, a small instrument is placed into the eye. It removes the vitreous and inserts the salt solution into the eye.
You may be able to return home soon after the vitrectomy. Or, you may be asked to stay in the hospital overnight. Your eye will be red and sensitive. After the operation, you will need to wear an eyepatch for a few days or weeks to protect the eye. You will also need to use medicated eye drops to protect against infection.
What research is being done?
The NEI is currently supporting a number of research studies in both the laboratory and with patients to learn more about the cause of diabetic retinopathy. This research should provide better ways to detect, treat, and prevent vision loss in people with diabetes.
For example, it is likely that in the coming years researchers will develop drugs that turn off enzyme activity that has been shown to cause diabetic retinopathy. Some day, these drugs will help people to control the disease and reduce the need for laser surgery.
What can you do to protect your vision?
The NEI urges all people with diabetes to have an eye examination through dilated pupils at least once a year. If you have more serious retinopathy, you may need to have a dilated eye examination more often.
A recent study, the Diabetes Control and Complications Trial (DCCT), showed that better control of blood sugar levels slows the onset and progression of retinopathy and lessens the need for laser surgery for severe retinopathy.
The study found that the group that tried to keep their blood sugar levels as close to normal as possible, had much less eye, kidney, and nerve disease. This level of blood sugar control may not be best for everyone, including some elderly patients, children under 13, or people with heart disease. So ask your doctor if this program is right for you.
For more information about diabetic retinopathy or diabetes, you may wish to contact:
American Academy of Ophthalmology
655 Beach Street
San Francisco, CA 94109-7424
(415) 561-8500
http://www.eyenet.org
American Optometric Association
243 Lindbergh Boulevard
St. Louis, MO 63141
(314) 991-4100
http://www.aoanet.org
American Diabetes Association
1660 Duke Street
Alexandria, VA 22314
(703) 549-1500
1-800-342-2383
http://www.diabetes.org
Juvenile Diabetes Foundation International
432 Park Avenue South
New York, NY 10016
(212) 889-7575
http://www.jdfcare.com
National Diabetes Information Clearinghouse
National Institute of Diabetes and Digestive and Kidney Diseases
1 Information Way
Bethesda, MD 20892-3560
(301) 654-3327
http://www.niddk.nih.gov
National Eye Institute
2020 Vision Place
Bethesda, MD 20892-3655
(301) 496-5248
http://www.nei.nih.gov
Prevent Blindness America
500 East Remington Road
Schaumburg, IL 60173
1-800-331-2020
(847) 843-2020
http://www.preventblindness.org
National Eye Institute
National Institutes of Health
NIH Publication No. 99-2171
March 2000
This educational material is provided by Dialog Medical.
© Copyright 2005 Dialog Medical
All Rights Reserved
The Eye Center
Call Toll Free 1.888.844.2020


