Printable Version (PDF)
Detachment of the retina from the outer supportive layer of the eye is a very serious condition. It is caused by a tear in the retina that allows the retina to separate from the eye wall. It is usually an emergency procedure when the tear is large or when the detachment does not involve the macula. In all cases it needs to be repaired. A surgery called scleral buckling with or without vitrectomy is necessary to preserve eyesight. Without surgery vision is usually completely lost.
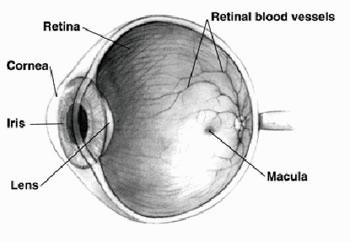
The retina is the light-sensitive tissue at the back of the eye. When light enters the eye, the retina changes the light into nerve signals. The retina then sends these signals along the optic nerve to the brain. Without retina function, the eye cannot communicate with the brain, making vision impossible.
Symptoms
Retinal detachment is often spontaneous or may result from trauma, severe nearsightedness, a thinned retina, or just the normal process of aging that causes small tears in the retina. The tears allow vitreous fluid to leak between the retina and the outer layers of the eye. When the fluid causes enough pressure and the layers split, the end result is retinal detachment. The symptoms may be one or more of the following:
Sudden vision changes, including:
- blurred vision
- flashes of bright light often at the outer edges of vision range (peripheral vision)
- blind spot(s) that are characterized as floaters or specks of dust floating in the eye
- curtain or shade blocking part of the vision
- near or total blindness in the eye
Treatment
Immediate surgical treatment is necessary – a surgical procedure called scleral buckling often in conjunction with cryotherapy. Laser or vitrectomy surgery is performed by an ophthalmologist in the operating room.
Scleral buckling surgery for retinal detachment is generally performed under local anesthesia. General anesthesia (the patient is asleep for the entire procedure) is less commonly used.
Before surgery begins, the eyelid will be pulled away from the eye with the use of a speculum and the eye not being treated will be covered with a patch. The surgeon will first treat the tear with either cryotherapy or laser photocoagulation.
Cryotherapy uses a probe that uses extremely cold temperatures to weld shut and repair the retinal tear. Photocoagulation is similar to cryotherapy in that it welds the retinal tear closed but instead of cold it uses laser treatment. A silicone band (scleral buckle) is sewn to the sclera (outside layer of the eye) so that it indents the eye wall to support the retinal tear(s). The silicone buckle will never be removed.
Various alternative methods may be used to ensure the retina properly re-attaches to the outer layers including injected gas inside the eye to help push the retinal tear closed and/or removing the vitreous jelly inside the eye to remove traction on the retinal breaks (vitrectomy).
The procedure may require an overnight stay in the hospital. As with any procedure, a risk of adversely reacting to the anesthesia always exists.
Other risks include:
- recurrence of retinal detachment
- development of glaucoma (increased pressure in eye)
- bleeding and/or infection inside or outside of eye
- red or painful eye
- loss of depth perception, blurring of vision, double vision, or blindness
- loss of eye
- tissue loss due to poor blood supply (anterior segment necrosis)
- swelling of layer under the retina (choroidal effusion)
- change in focus, requiring new spectacle or contact lenses (refractive changes)
- erosion of implant into the eye
- loss of contrast sensitivity
- infection around implant
- double vision
- developing cataract
- wrinkling of retina (macular pucker)
- swelling within retina (cystoid macular edema)
- distortion of vision, loss of peripheral vision (side vision)
Since the biggest risk of retinal detachment surgery is re-detachment of the retina, physical activity will be restricted after the surgery. To reduce the risk of infection, antibiotic drops will be instilled in the eye and should be continued until instructed to stop them. Recovery of vision may take several months and may never recover to pre-detachment levels. Vision is usually blurry immediately after surgery
Scleral buckling surgery has a greater than 80% success rate after the first surgery. With additional surgery, more than 90% of cases can be successfully reattached. It is important to understand that successful surgery does not necessarily correlate with good vision. The amount of visual recovery depends on how long the center of vision was detached before reattachment. It may take months before vision returns.
This educational material is provided by Dialog Medical.
© Copyright 2005 Dialog Medical
All Rights Reserved
The Eye Center
Call Toll Free 1.888.844.2020

